Understanding Progressive Supranuclear Palsy (PSP)
Progressive Supranuclear Palsy (PSP) is a rare and complex neurodegenerative disorder that is often misunderstood or misdiagnosed. As part of the atypical parkinsonian family of disorders, PSP shares some similarities with Parkinson’s disease—but it also has distinct characteristics that set it apart.
In this post, we’ll break down what PSP is, how it differs from Parkinson’s disease, common symptoms to watch for, and how therapy can help improve quality of life.
What Is Progressive Supranuclear Palsy?
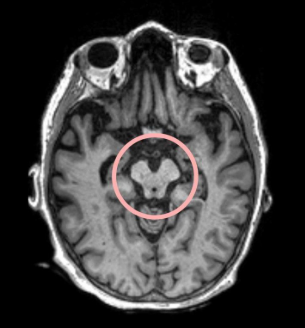
PSP is a neurological condition caused by the abnormal buildup of tau proteins in the brain. These proteins form tangles that damage nerve cells, particularly in areas like the brainstem, frontal lobes, cerebellum, and basal ganglia.
This degeneration affects movement, balance, vision, and cognition. While researchers are still working to understand the exact cause, most cases of PSP are not strongly linked to genetics.
PSP vs. Parkinson’s Disease: Key Differences
In its early stages, PSP is frequently mistaken for Parkinson’s disease (PD). However, there are several important differences:
Underlying cause: PSP is associated with tau protein buildup, while PD involves alpha-synuclein.
Falls: Individuals with PSP often experience early, unexplained backward falls. In PD, falls tend to occur later and are more often forward.
Eye movement: Difficulty looking up and down is a hallmark of PSP.
Speech and swallowing: These challenges appear earlier and are often more severe in PSP.
Tremor: Common in PD, but rare or absent in PSP.
Medication response: PSP typically shows little to no improvement with medications like levodopa.
Understanding these differences is critical for early and accurate diagnosis.
Common Symptoms of PSP
Symptoms of PSP can vary, but commonly include:
Slowness of movement (bradykinesia)
Small, cramped handwriting (micrographia)
Stiffness in the neck and upper body
A tendency to lean backward
A wide, stiff walking pattern
Sudden, unexpected falls
Difficulty with vision and eye movements (especially looking up and down)
Speech and swallowing challenges
Sleep disturbances
Changes in thinking, behavior, or personality
It’s important to note that there is no single test to diagnose PSP. Diagnosis is based on clinical evaluation, medical history, and symptom presentation.
How Therapy Can Help
While there is currently no cure for PSP, physical and occupational therapy play a crucial role in maintaining safety, independence, and overall function.
Therapy programs often focus on:
Maintaining independence with daily activities (ADLs)
Caregiver education and support
Eye movement exercises
Aerobic and strength training to reduce fall risk
Gait and balance training, including safe turning strategies
Assistive device training
Cognitive support and training
Early intervention and consistent therapy can make a meaningful difference in quality of life for individuals living with PSP.
Final Thoughts
PSP is a challenging condition, both for those diagnosed and their caregivers. Increased awareness and education are essential for early recognition and appropriate management.
If you or someone you know is experiencing symptoms consistent with PSP, seeking evaluation from a neurologist and a skilled therapy team can be an important first step.